Hospital staff train in new ER tents to prepare for surge in non-COVID-19 patients
Outside Toronto General Hospital’s emergency entrance, a stretcher appears quickly after a call for help.
Hundreds of ICU patients transferred between Ontario hospitals as COVID-19 admissions rise
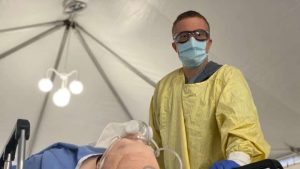
Around a dozen health-care workers in PPE practise responding to a simulated cardiac arrest. Some are observing the process as a medical mannequin is carefully lifted onto the stretcher, CPR is performed and nurses check for a pulse.
This situation isn’t new to hospital staff, but the environment is; they’re working in tents erected outside.
“These tents have been designed as waiting rooms and the purpose of them is to help people socially distance while waiting in the emerg so they can feel safer when they come here,” Dr. Alia Dharamsi explained. The physician at the University Health Network (UHN) is also the lead for the emergency department’s in-situ simulation program.
Recently, hospital staff, including registered nurses, nurse managers and educators, doctors and even security guards, have been running through various simulations to ensure any challenges in this new care setting — medical or environmental — are addressed.
Even though new COVID-19 cases and hospitalizations have been slowly going down, UHN says its emergency departments are still busy. As its hospitals anticipate a surge in patients who have been delaying care, staff are coming up with ways to create more space and ensure patients feel safe.

Last week, the team ran through simulations in the tent responding to a cardiac arrest and an overdose. Dharamsi says even though the tent is meant to be a waiting area, they want to be prepared to handle any potential medical emergencies. In the training process, they use various tools to communicate with staff inside and practise moving the patient safety.
She says they take notes on what they observe throughout the simulation.
“It can be as basic as the ground is uneven, which makes it difficult to push a stretcher. Or it can be as complex as how do we deliver CPR on a patient who is outside of our [emergency room],” she said.
“Then we write all of these challenges down, and we solve them one by one by one.”
Protocols on how to handle various challenges and changes in the emergency department throughout the pandemic have been written based on training sessions like these.
Sarah McDermid-Flabbi, an advanced-practice nurse educator at UHN, says the simulations are aimed at making both patients and staff feel safe and supported.
“It gives us an opportunity to do things in a light-hearted way; to learn in a safe environment, to make mistakes in a safe environment,” she said. McDermid-Flabbi added she’s been amazed by the number of times the team has adapted to new protocols, and the ways it’s brought her colleagues closer together.
“The pandemic has taught us to think on our feet time and time again.”
The ups and downs of ER visits
Dr. Sam Sabbah, medical director of UHN’s emergency departments, says at the peak of every wave of COVID-19, he sees a reduction in patients with other health issues.
“As the COVID activity comes down, people feel more comfortable seeking care for things that really they’ve been suffering from for a while,” Sabbah said.
“I anticipate as the vaccination ramps up and people feel more safe and comfortable, we will see a surge in activity in the emergency departments for many of the conditions that have been deferred throughout.”
Currently, he says, the hospitals are seeing a number of overdoses, patients experiencing mental health crises and victims of domestic violence and child abuse.

“All of those are the unwanted effects of being in a lockdown situation and people being confined indoors all the time,” he said.
In recent weeks, there have also been ER visits due to concerns over vaccine side effects, but Sabbah says the vast majority of the symptoms are minor.
“Unfortunately, because of all the concerns around the serious side effects, it’s caused a lot of distress to people who are seeking an assessment to ensure they’re not having the serious side effects.”
In addition to the waiting room tents, UHN and its partners have also created and expanded a virtual emergency room so people can access care from their homes and avoid a visit. But Sabbah wants people to know their emergency departments are safe.
“If you’re feeling unwell, you really should come and get checked out. Many conditions have a time sensitive complication rate so the longer you wait, the more likely complications will develop. We certainly would not want that for anyone.”
Despite these challenges, and the anticipated surge in non-COVID-19 patients in emergency rooms, Sabbah says he’s feeling hopeful about the future of health care in the province post-pandemic.
“It’s really taught us how to work together as a system more effectively than we’ve ever done before.”
Dharamsi anticipates the tents will be ready to use within the next few weeks.
“Ideally, this will remain a tent that never has a patient in it because that means we’re able to adapt our inside spaces,” she said.
“But we’ll be ready, if we do.”







Redes Sociais - Comentários