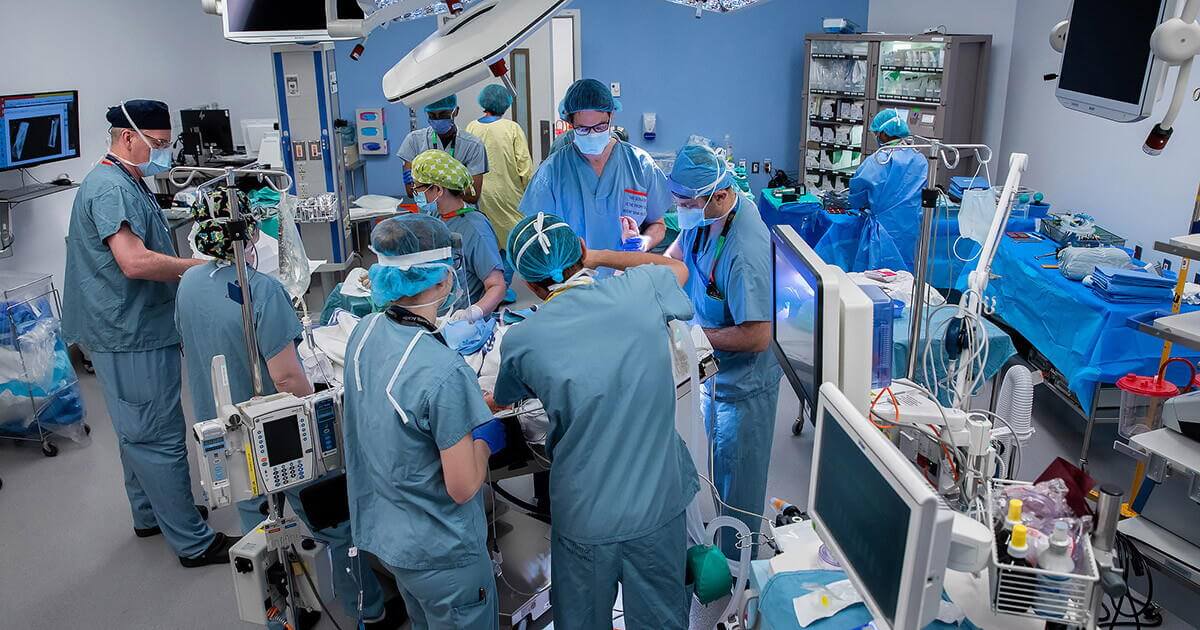
Frontline health care workers are suffering, and need to feel supported
If you got sick recently, tried to go to an emergency department and had to wait for hours before seeing a doctor, you are not alone. Before COVID-19, (2018 to 2019) most Canadians waited up to 3.9 hours in emergency to see a doctor for an initial assessment, according to the Canadian Institute for Health Information. By comparison, in Ontario, patients visiting emergency departments waited an average of 2.1 hours to see a doctor this May, and, on average, spent 20.1 hours waiting before being admitted, according to Health Quality Ontario. But the problem it’s similar in most of the Canadian provinces and despite the Premier’s asked for an increase in Canada Health Transfer (CHT) funding from 22% to 25%, Ottawa said no.
In the last weeks we realized that many hospitals across the country were forced to close their emergency rooms because of staff shortages. And now the concern is that the problem will get even worst during the rest of the summer, when the staff goes on vacation. Milénio Stadium tried to speak with the federal Minister of Health, Jean-Yves Duclos, to know more about the Liberal government plans to the health sector and received answers from Health Canada and the Public Health Agency of Canada.
Milénio Stadium: Signs of strain on the health care system have become increasingly apparent, from patients receiving treatment in hallways during pre-pandemic times, to waves of burnout and resource rationing throughout the COVID-19 crisis. The ER closures across the country are just the latest problem in the Canadian health care. How should the Canadian public healthcare system be in the post pandemic era?
Health Canada & Public Health Agency of Canada (PHAC): The Government of Canada recognizes that the pandemic has taken an emotional, mental and physical toll on health care workers, and that this can factor into their decisions about their future. Front-line health care workers are suffering, and need to feel supported. Therefore, to support mental health and well-being of our health workforce, Budget 2022 proposes to provide an additional $140 million over two years to the Wellness Together Canada (WTC) portal, which offers free, confidential mental health and substance use tools and services for front-line healthcare workers. These online services can also be accessed through PocketWell, WTC companion app. In the short term, key steps are being taken to help support the workforce.
MS: Considering that after social protection, health care is the Canadian government’s largest expense, Ottawa is considering allowing Canadians to pay for private healthcare services?
Health Canada & PHAC: Additionally, Budget 2022 proposes to provide $115 million over five years, with $30 million ongoing, to expand the Foreign Credential Recognition Program and help up to 11,000 internationally trained health care professionals per year get their credentials recognized and find work in their field. It will also support projects—including standardized national exams, easier access to information, faster time-lines, and less red tape— that will reduce barriers to foreign credential recognition for health care professionals. This is in addition to a $2 billion top-up to the Canada Health Transfer, provided to the provinces and territories, to reduce backlogs caused COVID-19. This will help to support the health and well-being of Canadians and those on the frontlines of our health care system.
MS: Canada has the fourth-lowest number of funded acute care beds per capita among countries in the Organization for Economic Cooperation and Development, according to the OECD, and the Commonwealth Fund ranked Canada’s health system second-last among 11 rich countries. Shouldn’t we be higher up in the rankings?
Health Canada & PHAC: The Government of Canada has been engaging with health system partners and stakeholders over recent months to further understand these gaps and needs, and work collaboratively to identify concrete solutions to address the challenges and to deliver results for Canadians, their families and for our health care workers. The Government of Canada continues to work with provincial and territorial governments and stakeholders to support the pandemic response, and to improve Canada’s health care system, including solutions to address the health human resource crisis the sector is currently facing, so that it can meet the needs of Canadians and the health workforce.
MS: Primary-care providers address most health concerns for their patients, offer preventive care to keep people healthy, and when necessary, co-ordinate referrals to specialized services, such as surgery. But about 15 per cent of Canadians do not have a family doctor. What is the Canadian government’s plan to fill more family doctor training positions across the country?
Health Canada & PHAC: We are committed to protecting and strengthening Canada’s publicly funded health care system and we welcome the ongoing dialogue with stakeholders on important health policy priorities, and looks forward to continued collaboration with them on these issues. Canadians deserve access to accessible, high-quality health care, and continued collaboration with provinces and territories, who have the responsibility for matters related to the administration and delivery of health services, including health workforce planning and management, is indispensable to address pressing health workforce challenges. Action has been taken to address key concerns voiced by health care providers. A safe working environment is critical to support the retention of health care workers, which is why we have made amendments to the Criminal Code (under the former Bill C-3), in order to ensure health care workers are safe and free from threats, violence and harassment.
MS: Provinces have been asking for a 13% increase in health care funding. Why is Ottawa not open to this request?
Health Canada & PHAC: To support health care workers’ financial needs and address supply and retention issues in rural and remote communities, Budget 2022 announced $26.2 million in funding to increase the forgivable amount of student loans for doctors and nurses who practice in rural and remote communities. This will mean up to $30,000 in loan forgiveness for nurses and up to $60,000 in loan forgiveness for doctors working in underserved rural or remote communities. Also, Budget 2022 proposes expanding the list of eligible professionals under the program in order to help bring more health care workers to the communities that need them most. The Government is also hiring a Chief Nursing Officer, which will bring nursing issues to the forefront federally and support work with provinces and territories, stakeholders, and regulatory bodies.
Joana Leal/MS







Redes Sociais - Comentários