Opioid overdoses spike in homeless shelters despite Toronto’s harm-reduction program
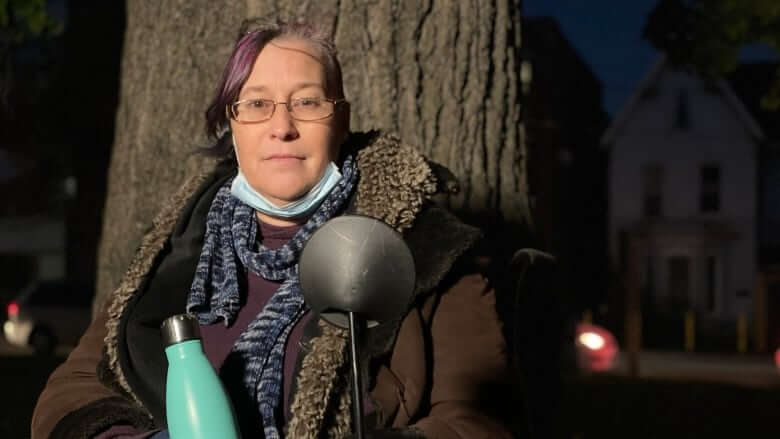
Jennifer Jewell has lived in one of Toronto’s shelter hotels for the past year.
In her time there, the 51-year-old says she has regularly seen overdoses among the other residents, just some of the 610 suspected overdoses in city shelters in the first six months of 2021, according to a City of Toronto dataset that can be found on its open portal. Of those, 26 have been fatal.
“There’s way too many deaths,” Jewell said.
“At least one death a week in the last month … And there aren’t [enough] mental health support services. People lose their friends to death all the time and there’s nothing for them.”
It’s a staggering increase over the same time period in 2020, when the city documented fewer than 10 fatal overdoses in its shelters.
The spike comes despite efforts by the city to boost overdose prevention strategies in its shelters. In December, the city launched the Integrated Prevention and Harm Reduction Initiative (iPHARE). The program provided $7 million to partner agencies to implement a range of harm reduction supports, such as enhanced mental health efforts and a limited number of supervised consumption sites.
And yet, the number of overdoses in shelters has continued to climb.
Distancing can be deadly for drug users, advocates warn
Some advocates working on the front line say moving people from encampments into hotel shelters may have made the overdose crisis worse.
Lorraine Lam, an outreach worker at Sanctuary Toronto, a non-profit that works with the unhoused, said encampments offered community and safety to residents.
“A lot of people who are living outside are first responders. They are there way before paramedics,” she said. “If one person goes down, others are able to be there … to literally save people’s lives.”
However, in city-run hotel shelters many residents live in relative isolation due to physical distancing measures. Lam said that can be extremely dangerous for drug users.
“It’s like the golden rule: never use alone,” Lam said. She also pointed to the need for more safe consumption sites at city shelters.

Diana Chan McNally, the training and engagement coordinator at the Toronto Drop-In Network, agrees.
“We’ve been advocating to have supervised consumption sites placed in every single shelter hotel,” she said.
Currently, only three out of 26 of the city’s temporary shelters have safe consumption sites, operated by Toronto Public Health. Opening more sites isn’t up to the city alone, however. It has to apply for an exemption from the province, McNally said.
The city says it has requested urgent provincial assistance.
In an emailed response to CBC News, Ontario’s Ministry of Health stated it will continue to work with its municipal partners to combat the opioid crisis and pointed to $30 million in funding it has provided to operate 21 consumption and treatment sites across the province.
In addition to more safe consumption sites, both Lam and McNally also identified peer witnessing programs as a way to discourage isolated drug use.
“When you’re using drugs, you don’t necessarily want to go into a semi-clinical setting,” McNally said.
“Allowing people to support each other in their rooms, not necessarily in a dedicated site, would go a long way to mitigating the level of overdose we’re seeing in shelter hotels.”

Too many residents, too few staff
Staffing has also been a problem contributing to the rising number of overdoses, according to Lam.
“I don’t think there’s enough staff who are adequately trained,” she said. She attributes that to the speed at which temporary shelters needed to open in response to COVID-19.
“We know that it takes a lot of years of doing this to really be able to respond adequately,” Lam said. “I’ve had people tell me they witnessed overdoses and staff are just standing back because they don’t know what to do or they refuse to respond.”
She suggested hiring shelter residents themselves to respond when an overdose occurs.
“Those are going to be the most effective people in understanding how harm reduction works,” Lam said.
In an emailed statement to CBC News, the city noted its shelter directive asserts that, “all program staff on each shift will be trained in overdose prevention, recognition and response, including the administration of naloxone,” a drug that can block the effects of opioids and help reverse overdoses.
“All clients will be offered a naloxone kit and training upon admission. Shelter providers will ensure naloxone kits … are available at all sites for staff and resident use,” the statement reads.
Additional calls for safe supply
Dr. Andrew Bond, medical director at Inner City Health Associates, said one of the top priorities should be to ensure a safer supply of drugs.
“We have a huge amount of tainted drug supply right now,” he said. “When the scale is so substantial, it’s not that people are using inappropriately or using in dangerous ways. It’s just they’re using substances that happen to be so toxic that almost any dose can kill them.”
With overdoses still on the rise, Jewell said more needs to be done faster.
“They need to do something about this now, because … a lot of these deaths are completely preventable,” she said.
“And we can’t wait anymore because too many of us are dying.”








Redes Sociais - Comentários