Breast cancer screening guidelines based on flawed Canadian study, new paper says
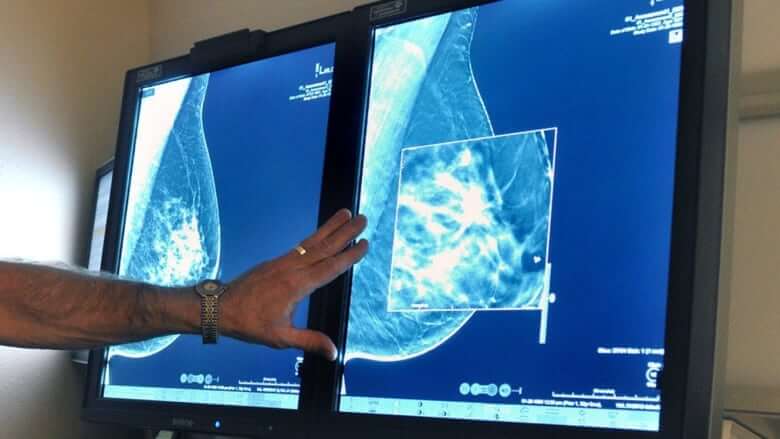
A new paper calls into question a decades-old Canadian study that has informed breast cancer screening guidelines for women in their 40s around the world, which generally do not recommend a yearly mammogram.
The commentary — co-written by researchers at The Ottawa Hospital, Sunnybrook Research Institute in Toronto, the University of British Columbia, the University of Alberta and Harvard Medical School — will be published inthe Journal of Medical Screening this week.
It specifically points to randomization issues with the Canadian National Breast Screening Study (CNBSS), originally conducted in the 1980s, which involved tens of thousands of women and eventually took place in 15 different urban centres across the country.
The randomized trials set out to determine whether or not screening helped save women’s lives. In the first study, women aged 40 to 49 were randomly assigned to receive mammograms or placed in a control group where they had a single physical exam, with all participants followed up with for several years.
Over the course of the study, there were 38 deaths from breast cancer in the mammography group and 28 among those who didn’t receive mammogram screenings.
As a result, Canadian researchers concluded that annual screening in women aged 40 to 49 at average risk does not reduce breast cancer mortality any more than a physical exam.
The study has gone on to inform guidelines both here and around the world. The most recent guidelines issued by the Canadian Task Force on Preventive Health Care still do not recommend screenings for women in that age group.
A key issue of earlier screening is the risk of false positives and over-diagnosis. There are lumps that aren’t cancerous or harmful to women, but if discovered, would require a biopsy.
Experts have warned any kind of breast cancer treatment — whether it be radiation, chemotherapy or surgery — may carry harm.
New evidence
But the CNBSS had several problems, according to Dr. Jean Seely, co-author of the new paper and a professor of radiology at the University of Ottawa and head of breast imaging at The Ottawa Hospital.
She and her co-authors are calling for mammograms for women aged 40 or older, should they want them.
Seely said there is now “conclusive confirmation” the CNBSS was conducted — particularly in some trial locations — with women who weren’t randomly assigned.
When interviewing 28 staff members who worked on the original study, some confirmed there were multiple instances in which women with detectable lumps, who were pre-screened by a nurse, were in fact purposefully placed in the mammography group, she said.
“I was astonished. I did not expect to find such clear, clear evidence of what was going on,” Seely said. “Then I think my next reaction was anger. How could this have been allowed?”
The paper adds to the long-standing debate over the quality of the studies since they were first published and whether women in their 40s should be regularly screened.
Since the ’90s, radiologists and researchers have raised concerns about the inclusion of women with advanced cancers in the study, the quality of the screening and the factors used to determine if mammographies were beneficial for that age group.
Experts have mostly suspected issues with the randomization, which they say would’ve skewed the findings.
An investigation into these suspicions was done by external experts in the 1990s after the first results of the CNBSS were published.
The resulting paper said it “failed to uncover credible evidence” that the randomization was subverted in any way. Its authors further said that even if there had been acts of subversion, they would have been “few in number” and “alterations could have had only a trivial effect on the study findings.”
Results would be different, experts argue
Still, some experts aren’t convinced; the new paper concludes that results of the trial would have changed with the seven instances of women with lumps from the mammography group sent to the usual care group.
Seely said she’s hopeful this new evidence will lead to change.
“I think probably the most personal challenging moments that I have in my practice are when I see a woman in her 40s who presents with an advanced breast cancer,” she said.
More often than not, Seely said, those women were told by their family doctors they shouldn’t be screened because of their age. “On a personal level, as a professional, I find this very, very difficult,” she said.
According to the Canadian Cancer Society, while women aged 50 and older have higher rates of breast cancer diagnosis, there’s a higher rate of mortality for women between 30 and 49.
Women in that age range consist of 17 per cent of all cancer deaths in Canada. That’s compared to women aged 50-69, who represent just eight per cent of cancer deaths.
Lead investigator defends study
Many other experts, including the principle investigators of the CNBSS, continue to defend the study.
“We had a great deal of understanding of what could go wrong with randomization and we took a great deal of care to ensure it didn’t apply in the National Breast Screening Study,” said Dr. Anthony Miller, a professor emeritus at the Dalla Lana School of Public Health at the University of Toronto, who led the study.
Miller, who has seen a copy of the new paper, denies the possibility that any women were not placed randomly within the trials. There were extensive quality-control measures in place to maintain the integrity of the study, he said.

Nurses were only in place to inform participants about the study and get their consent, he said, and any examinations happened after a woman had been randomized.
At that point, Miller said, excluding women who may have had palpable lumps “would indeed falsify the results of the study.”
CNBSS considered gold standard
Miller is not alone in his defence of the CBNSS. While its authors say their work has been under attack for decades, the CBNSS has withstood years of skepticism and challenges.
The study has been hailed by many around the world as the gold standard in breast cancer screening research. In 2019, a 25-year followup to the study was named one of the British Medical Journal’s Top 5 research papers of the last decade.
Compared to a number of other breast cancer screening trials, it would be difficult to find one as well documented and well run as the CNBSS, according to Dr. Karsten Jørgensen, acting director of the Nordic Cochrane Centre, which reviews medical trials, including those on breast cancer screening.
Canada’s trial results also align with other reputable studies around the world, which show no benefit to early screening, Jørgensen said.
“There’s always room for interpretation. There’s also always pitfalls. There’s always limitations with the trials — but that’s why we do systematic reviews and these types of meta-analysis,” said Jørgensen.
“Much of this is down to interpretation and which results should you trust.”
New findings being considered
Seely and her fellow researchers have raised their concerns about the CNBSS to the University of Toronto and the Canadian Medical Association Journal, both of which were involved in the original study.
In a statement, the university’s office in charge of research, oversight and compliance said it “places a high value on research integrity” and is “reviewing the concerns raised by a group of individuals and has been in touch with them.”
The university did not specify the scope or timeline of its review, only that it will “get back to them with our next steps.”
“CMAJ will co-operate with the university office’s process fully and will await the office’s report on the outcome of the review before deciding if any further action is needed,” Dr. Kirsten Patrick, interim editor-in-chief of the journal, wrote in her own statement.
She did not provide any further comment.
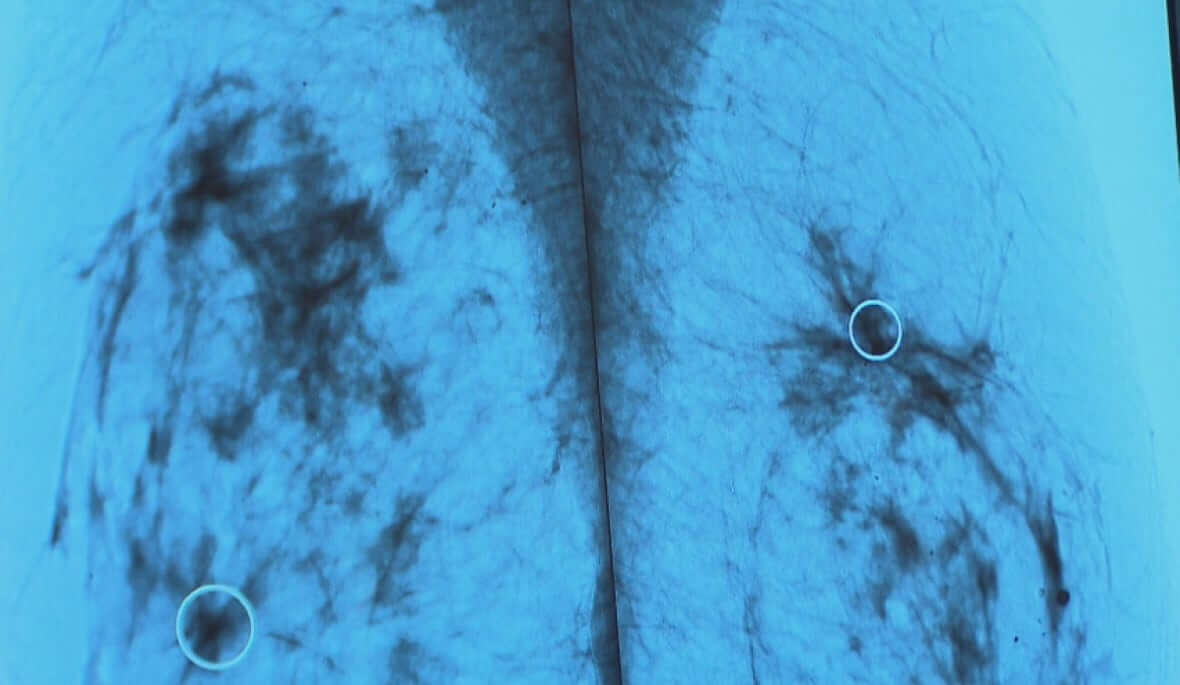
Unlikely guidelines will change
The Canadian Task Force on Preventive Health Care says it is unlikely it will consider changing the country’s current guidelines on breast cancer screening to include women in their 40s.
In a written response to CBC, the task force defended its guidelines, saying it “conducts rigorous, detailed evidence reviews” when formulating them.
“Our guidelines, including those on breast cancer screening, have been recognized as the best in the world,” said Dr. Brenda Wilson, co-chair of the task force.
Wilson wrote “the best available evidence” is used to inform the guidelines. When there are changes to that evidence, she said the task force “updates a full review of the body of evidence, including any new evidence.”
The task force doesn’t comment on individual studies or opinion pieces without doing that review, she said.






Redes Sociais - Comentários